Mapping community health services in Mukuru, Kenya
By Jane Wairutu, Eva Muchiri and Jackline Waithaka
Kenya’s health sector has set the stage for major improvements with a strategic focus guided by Vision 2030. It aims to transform Kenya into a globally competitive and prosperous country. However the burden of ill-health continues to be felt nationwide, particularly among the urban poor. Mukuru belt has the largest slum settlements in Nairobi. A community mapping exercise was conducted to provide new information on who is under-served by health services and where greater focus is needed. This blog gives insights into how the mapping was conducted and the greater contribution makes to improving the community health sector.
Mukuru Special Planning Area
Mukuru was declared a Special Planning Area (SPA) in August 2017 because residents not only faced constant evictions but also did not have access to basic services at an affordable cost. Often, they were paying five times as much as the residents of formal areas for health, water, sanitation and education services. Being declared an SPA paved the way for the creation of an Integrated Development Plan for all sectors through a participatory process that was community led. One of the main objectives of the SPA is devising ways to promote the health and safety of Mukuru residents.
Profiling and mapping Mukuru
 In Kenya, the health system is divided into six levels – Level One is the community level. At this level a combination of paid (Community Health Assistants) and unpaid (Community Health Volunteers) workers deliver care. They are attached to a Community Health Unit (CHU). Each CHU is responsible for 100 households that are assigned one Community Health Volunteer (CHV). The main roles of the CHVs are to: support people, households and communities to promote health; provide simple health interventions; refer patients with more complex needs to health facilities; and collect data for their supervisors to inform health planning. They are the frontline of the health system.
In Kenya, the health system is divided into six levels – Level One is the community level. At this level a combination of paid (Community Health Assistants) and unpaid (Community Health Volunteers) workers deliver care. They are attached to a Community Health Unit (CHU). Each CHU is responsible for 100 households that are assigned one Community Health Volunteer (CHV). The main roles of the CHVs are to: support people, households and communities to promote health; provide simple health interventions; refer patients with more complex needs to health facilities; and collect data for their supervisors to inform health planning. They are the frontline of the health system.
SDI Kenya used various techniques including satellite imagery to map the physical coverage of all CHVs and spatially identifying the unserved pockets and the number of CHUs. An individual profiling survey tool was developed and it focused on issues like CHV level of training, experience and level of satisfaction.
What did we find?
Health Facilities
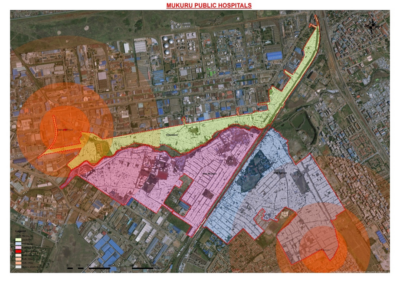 A profiling of health facilities had initially been carried out by the Federation, CHVs and organizations within the Mukuru SPA Health Consortium. They mapped 206 health facilities which were both private and publicly owned. But only four of them had government support. The state owned facilities are located in Viwandani and Imara Daima, one is a dispensary, while the other is a Health Centre. Currently the two facilities do not provide a 24 hour service for all the residents, they only provide outpatient services and limited emergency care. The Health Centre provides maternity care for normal deliveries, laboratories, oral health and referral services. In addition, the Health Center offers preventative care and promotes good health practices to improve well being.
A profiling of health facilities had initially been carried out by the Federation, CHVs and organizations within the Mukuru SPA Health Consortium. They mapped 206 health facilities which were both private and publicly owned. But only four of them had government support. The state owned facilities are located in Viwandani and Imara Daima, one is a dispensary, while the other is a Health Centre. Currently the two facilities do not provide a 24 hour service for all the residents, they only provide outpatient services and limited emergency care. The Health Centre provides maternity care for normal deliveries, laboratories, oral health and referral services. In addition, the Health Center offers preventative care and promotes good health practices to improve well being.
The majority of residents in Mukuru get their health care from private facilities. Out of the 206 health facilities profiled, 60 (29%) were registered while 140 (71%) were not registered and operated illegally.
Community Health Services
 During the mapping 388 CHVs were profiled (82%) were women and (18%) were men. The majority had two to three years of experience. On the levels of training, 363 (94%) of the CHVs said that they had undergone both basic and technical training. The training was supported by the County and National Government with support from various faith-based organisations, NGOs and CBOs working in Mukuru. These organisations included Access Afya, APHRC, AMREF and UNICEF. More than half the CHVs referred patients to the existing public health facilities.
During the mapping 388 CHVs were profiled (82%) were women and (18%) were men. The majority had two to three years of experience. On the levels of training, 363 (94%) of the CHVs said that they had undergone both basic and technical training. The training was supported by the County and National Government with support from various faith-based organisations, NGOs and CBOs working in Mukuru. These organisations included Access Afya, APHRC, AMREF and UNICEF. More than half the CHVs referred patients to the existing public health facilities.
During the mapping process the CHVs were assisted by the Community Heath Assistants who helped them in understanding the geographical areas they cover while seeking to capture details of the service providers they refer patients to. The data collection process, which fed into the upsurge in demand for health information, deployed over 40 trained CHVs from the three settlements within the SPA.
Opportunities for change
In Mukuru, as in other informal settlements in Nairobi, residents face extreme health challenges. The CHVs also face challenges. These include inadequate numbers of workers to meet the needs of the population they have to cover, interrupted supply of commodities, lack of access to specialized services, inefficiency and ineffectiveness of among other health care staff and weak implementation of the Community Health Strategy.
Spontaneous responses from the survey provided insights into the dynamics of the health care system at the settlement level paving the way for deeper understanding.
Our job entails service and service requires patience. It requires patience to serve the community even in instances where, as health practitioners, we may lack the proper working tools and facilitation to enable us conduct our activities effectively. Christine, Wape Wape
The survey further revealed the burden of cholera, because of poor sanitary conditions and unreliable garbage collection, which was considered an urgent issue among CHVs. The data obtained from the survey pointed to specific shortfalls and helped determine areas to focus on in a bid to streamline the sector.
The data will help us functionalize more Units in regards to the boundary gaps that came out from the data collection exercise. Lucy, Community Health Assistant, Viwandani
Implementation of the mapping exercise was a significant but doable undertaking, one that went further to map where services are provided to address deficiencies in service provision and generate the much-needed evidence to refine the health sector response in Mukuru.






